Trauma and Stressor Related Disorders
Major psychological stress involves a threatening event or loss. The stress response involves physical, emotional, and psychological components.
- Response to stressors
- Emotional responses: threat → fear; Loss → sadness
- Physical symptoms: autonomic arousal/ fatigue
- Psychological responses
- Conscious: avoidance behaviour
- Unconscious: denial OR dissociation
- Trauma and stressor-related Disorders
- Reactive attachment disorder
- Disinhibited social engagement disorder
- Acute Stress Disorder
- Posttraumatic stress disorder (PTSD)
- Adjustment Disorder
Reactive Attachment Disorder
Disorder whereby children (< 5 years) are unable to form healthy attachments (particularly with their primary caregiver).
- Causes
- Insufficient care (neglect, deprivation)
- Repeated changes of primary caregiver
- Limited opportunities to form stable/selective attachments (absenteeism, institutions with high child-to-caregiver ratio)
- Risk factors
- Living in an orphanage
- Institutional care
- Prolonged hospitalization
- Frequent changes in caregivers
- Extreme neglect/poverty
- Physical, sexual, or emotional abuse
- Post-partum depression in the mother
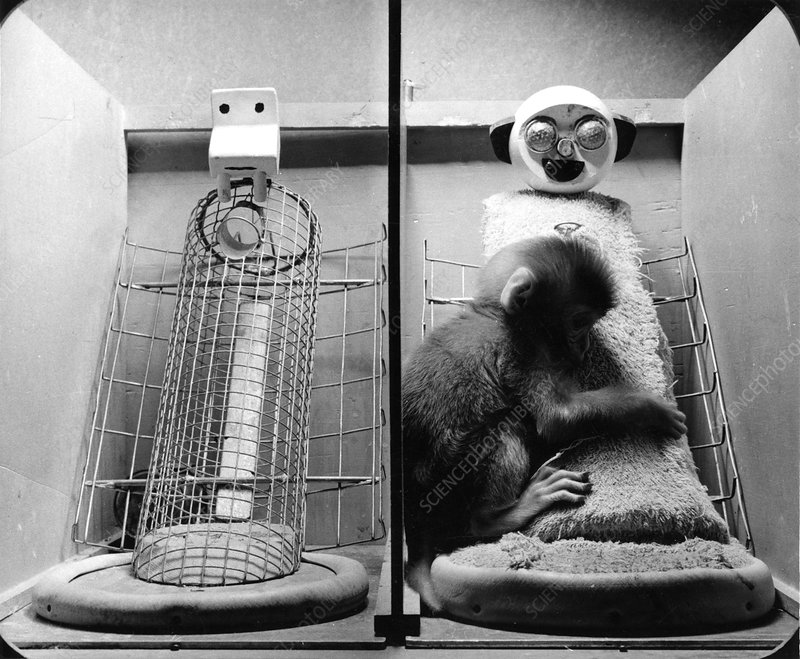
- Attachment theory
- John Bowlby: early separation of infants from their mothers has a severe negative effect on children’s emotional and intellectual development
- Mary Ainsworth: interaction between mother and baby during the attachment period significantly influences the baby’s current and future behaviours
- Sx
- Emotionally withdrawn behaviour towards the adult caregiver
- not seeking comfort when distressed
- not responding to comfort when provided)
- Social and emotional disturbances
- Limited social and emotional responsiveness
- Limited positive affect
- Episodes of unexplained irritability, sadness or fearfulness (evident during non-threatening interactions with adult caregiver)
- Emotionally withdrawn behaviour towards the adult caregiver
- Specifiers for diagnosis
- Persistent: The disorder has been present for more than 12 months
- Severe: The child manifests all Sx of the disorder, each Sx manifesting at high levels
- Differentials
- Autism Spectrum Disorder
- Intellectual Developmental Disorder
- Depressive Disorder
- Treatment
- Psychotherapy
- Dyadic developmental psychotherapy: to enable the child to maintain and affectively attuned relationship
- Attachment therapy
- Play therapy
- Paint therapy
- Child-parent intervention
- Behavioural Management Therapy: to treat behavioural Sx (more of a band-aid)
- Psychotherapy
Disinhibited Social Engagement Disorder
Characterized by a child who actively approaches and interacts with unfamiliar adults in an impulsive, incautious, and overfamiliar way (basically the opposite of reactive attachment disorder). Management is the same as RAD.
- Cause
- Serious social neglect (before 2 years)
- Sx
- Readily approaches strangers (w/o fear and excessive familiarity)
- Readiness to hug and accept comfort, food, or toys from unknown persons
- Diminished or absent checking back with adult caregiver after venturing away
- Willingness to go off with unfamiliar adults with minimal or no hesitation
Acute Stress Disorder and Post Traumatic Stress Disorder (PTSD)
Two peas in the same pod. Same symptoms. Characterized by severe symptoms of fear and avoidance following a threatening event (threatening = problematic to the patient’s psychological stability) or loss. Diagnosis is clinical. Watch for depressive symptoms which may progress to MDD, and increased risk of suicide.
Risk of developing PTSD after a traumatic event 8-13% (men) and 20-30% (women). Lifetime prevalence 7.8% (M:F = 1:2)
- Stressors associated with higher rates of PTSD
- Rape
- Torture
- Prisoner of war
- Populations at risk of developing PTSD
- Single
- Divorced
- Widowed
- Socially withdrawn
- Low SES
- Key symptoms
- Flashbacks/nightmares (pervasive and problematic)
- Avoidance
- Anxiety
- Emotional numbing
- Hyperarousal/reactivity
- Sx for less than one month
- Acute stress disorder
- Sx for more than one month
- PTSD
- Specifiers for diagnosis
- With dissociative Sx (Depersonalization, Derealization)
- With delayed expression (full Dx criteria not met until at least 6 months after the event)
- Treatment
- Benzodiazepines: acute symptoms (esp. when having flashbacks
- SSRIs
- Group therapy (Some patients will have “survivor guilt” so group therapy helps them come to terms with that)
- Cognitive Behavioral Therapy (CBT)
- Eye movement and desensitization and reprocessing (EMDR)
Adjustment Disorder
Maladaptive symptoms of depression, anxiety, or behavioural changes that follow a distinct stressor or life change, less than 6 months after the event.
- How can adjustment disorder manifest in kids
- As regression (eg. child will wet bed; remember that children do not manifest depression the same way as adults)
- Differentials
- Acute stress disorder/PTSD: symptoms will follow a significant threat or involve flashbacks/nightmares, panic symptoms, and/or avoidance
- MDD: symptoms will involve > 5 SIG E CAPS sx for > 2 weeks
- In brief psychotic event, Schizophreniform disorder: involves psychotic symptoms
- Treatment
- Psychotherapy
- SSRIs
