Changes from DSM-IV to DSM-V
- Sleep disorders related to another mental disorder/medical condition have been removed from DSM-V (e.g. insomnia d/t depression, which makes the diagnosis of sleep disorder more specific)
- Primary insomnia has been renamed insomnia disorder (avoids the differentiation between primary insomnia and secondary insomnia, which is technically not a sleep disorder according to the DSM-5)
- DSM V distinguishes narcolepsy from other forms of hypersomnolence (the basis of narcolepsy has been found)
- Breath-related sleep disorders
- Obstructive sleep apnea-hypopnea
- Central sleep apnea
- Sleep-related hypoventilation
- Circadian rhythm sleep-wake disorders
- Advanced sleep phase syndrome
- Irregular sleep-wake type
- Non-24-hour sleep-wake type (90% in completely blind patients)
- The jet-lag type has been removed
- REM sleep behaviour disorder and restless leg syndrome are recognised as independent clinical entities (primary diagnoses) rather than collapsing under the sleep disorders NOS category
Organisation of Sleep
Brain wave patterns
- Beta waves
- Awake
- Alpha waves
- awake-drowsy/sleepy/relaxed
- Theta waves
- light sleep (NREM 1)
- K waves and sleep spindles
- Sleep NREM 2
- Delta waves
- Deep Sleep (NREM 3 and NREM 4)
Stages of Sleep
- Hypnogram
- The time between REM episodes decreases
- Duration spent in REM increases
- Stage 4 sleep is the longest stage
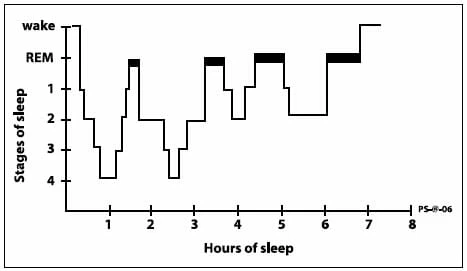
- NREM sleep (75%)
- Body active (muscular tone), High muscular tone, Brain inactive (no conscious thoughts), No eye movement
- NREM 1: theta waves, 5%
- NREM 2: K waves and sleep spindles, 45%
- NREM 3: delta waves appear, 12%
- NREM 4: delta waves continue, 13%
- REM sleep (25%)
- Body inactive, Brain active (dreams), Rapid eye movement, No muscular tone
- Sawtooth waves
- Length of REM episodes increases through the night
- The frequency of REM increases through the night
- Delta sleep
- NREM 3 and NREM 4. Have delta waves
- Hardest to arouse
- Duration decreases with age
- REM latency
- Time measured between falling asleep and the onset of REM. The average is 90 minutes
- Shortened in:
- Depression
- Narcolepsy
- Sleep latency
- The average time it takes to fall asleep is 15 minutes
- Lengthened in:
- Insomnia
- Shortened in:
- Narcolepsy
Neurochemicals involved in sleep
- Serotonin (Increased)
- Involved in sleep initiation
- Hence, some SSRIs will make you drowsy
- Acetylcholine (increased)
- Involved in REM sleep
- Norepinephrine (decreased)
- Involved in REM sleep
- Dopamine (increased)
- Involved in arousal and wakefulness (but is increased during sleep)
- Dopamine agonists (Parkinson’s agents – bromocriptine, pramipexole): produce arousal, making it harder to sleep
- Dopamine antagonists (Antipsychotics – haloperidol, risperidone, etc): reduce arousal, making it easier to sleep (sedating)
- Alcohol and barbiturates (reduce REM sleep)
- REM rebound: increased REM sleep on acute withdrawal
Relationship between depression and sleep
- Reduced REM latency
- A greater percentage of sleep time is spent in REM
- A lower percentage of time spent in Delta sleep (NREM 3-4)
- Multiple awakenings throughout the night
- Early awakening
Sleep Changes with Age
- Less time spent sleeping overall (6-7 hours of sleep by the 60s)
- Delta sleep (NREM 3-4) decreases until vanishing
- Time spent in REM decreases
- The majority of the time, sleeping will be in NREM 1-2
Insomnia (initiation Phase)
Insomnia is characterised by an inability or difficulty initiating sleep OR staying asleep, which affects the patient’s level of functioning or leads to daytime sleepiness. It is very common and may be chronic or situational.
- Symptomatic occurrence
- Major depressive disorder
- Mania (has decreased need for sleep, will not have daytime sleepiness)
- Anxiety
- Comorbidities
- Anxiety disorders (GAD)
- Differentials
- Any psychiatric disorder that may cause insomnia (depression, anxiety, and mania): these will not have daytime sleepiness
- Hyperthyroidism: will not complain of daytime sleepiness. Have symptoms such as tremors, weight loss, and decreased appetite
- Gastroesophageal reflux disease
- Treatment
- Behavioural modification (Sleep hygiene)
- Benzodiazepine-like drugs (Zolpidem)
- Sleep hygiene
- Keep the room as dark as possible – no television with closed curtains)
- Environmental control – comfortable sleeping temperature, clothes or lack thereof
- Minimise distractions – keep work material out of the bedroom
- Do not work, read, or watch television in bed. The bed should be reserved for sleep & sex only.
- Avoid daytime naps
- Avoid eating 1-2 hours before sleep
Obstructive Sleep Apnea (all phases)
Obstructive Sleep Apnoea is characterised by cessation of airflow through the respiratory passages during sleep (associated with snoring with long pauses). Diagnosed on a formal sleep study.
- Risk factors
- Obesity
- Male
- High “Mallampati” score
- Signs and symptoms
- Daytime sleepiness
- Headaches in the morning (acidotic, low pO2)
- Dry mouth (use mouth to breathe)
- Dry nasal passages
- Sleeping partner complains of loud snoring or restlessness
- Treatment
- Home CPAP
- Weight loss (diet and exercise)
- ENT surgery (if indicated, class III and class IV Mallampati)
Parasomnias
Sleepwalking
Patients who sleepwalk may perform mental activities such as opening cupboards, opening windows, turning things on/off, etc. It occurs during NREM 3-4 when the body is active, has muscle tone and has no conscious activity.
It is common in men and starts at a young age
- Patient history
- Can go back to bed OR Awaken during the walk and become confused
- Agitated when woken by someone else
- Treatment
- Ensure safety, e.g. alarms
- Benzodiazepines – reduce the length of NREM 3-4, hence reducing the frequency and duration of sleepwalking
Night terrors
Night terrors are primarily a paediatric disorder. They are characterised by inconsolable, loud shrieking and general fearful demeanour while sleeping. The patient may appear to be awake but is sleeping. It remits in minutes, with the patient immediately returning to sleep and having no memory of the event. It occurs during NREM 3-4.
- Treatment
- Rarely indicated
- Benzodiazepines if frequent
Nightmares
Nightmares are unpleasant dreams. They occur during REM, and the memory of the episode is usually intact.
- Comorbidities/Occurrence
- PTSD
- Depressive mood
- Anxiety disorders (especially anticipatory anxiety)
- Treatment
- Generally not indicated
- Alpha-blocker (Prazosin; especially in PTSD)
- TCA (Imipramine)
Narcolepsy
Narcolepsy is a disorder of REM, where the patient complains of excessive daytime sleepiness accompanied by sleep attacks and sudden loss of muscle tone (cataplexy). Hypnagogic and hypnopompic hallucinations are common – these never qualify as psychotic; they are quite common in normal individuals, too. The diagnosis is confirmed if the patient has had symptoms for ≥ 3 months.
- Cataplexy
- Pathognomonic for narcolepsy
- Triggered by: intense emotions, loud sounds, flash of light
- Treatment
- Forced naps at regularly scheduled times(s) throughout the day.
- Stimulants (Modafinil) to increase wakefulness
- TCAs (imipramine) for cataplexy prophylaxis (suppresses REM)
Sleep Paralysis
Sleep paralysis is a common condition characterised by transient paralysis of skeletal muscles, which occurs when awakening from sleep or, less often, while falling asleep. It is thought to be related to the paralysis that occurs as a natural part of REM (rapid eye movement) sleep. Sleep paralysis is recognised in a wide variety of cultures
- Signs and symptoms
- Paralysis: occurs after waking up or shortly before falling asleep
- Hallucinations: images or sounds that appear during the paralysis
- Treatment
- Clonazepam
