Last updated:
November 18, 2024
- Pathophysiology of excess scar production during wound healing
- Excessive scarring results from an overabundance of collagen production by fibroblasts in the wound
- There is increased production of:
- Certain isoforms of TGF-B (Primary mediator) – TGFB1 and B2 increase angiogenesis (proliferation) and collagen deposition (maturation); also prevents collagen breakdown by inhibiting metalloproteinases (collagenase) and upregulating tissue inhibitors of metalloproteinase
- Connective tissue growth factor (downstream signaling factor of TGF-B)
- PDGF
- Tissue inhibitors of metalloproteinases
- Decreased production of
- Fibroblast growth factor (FGF)
- Metalloproteinases (collagenases)
- IL-10
- Treatment options for keloids and hypertrophic scars
- First line: Silicon gel
- +/- pressure garment
- +/- steroids
- Second line: Steroids
- +/- silicon
- +/- cryotherapy
- +/- 5-FU
- Third line: Surgery
- +/- steroids
- +/- radiation therapy
- +/- 5-FU
- First line: Silicon gel
| Excess healing | Description |
|---|---|
| Excessive scarring | Excess proliferation of fibroblasts and collagen due to dysregulation of the proliferative and maturation stage |
| Hypertrophic scar | Excess proliferation of fibroblasts and collagen leading to a raised scar that does not grow beyond the boundaries of the original lesion |
| Keloid | Excess proliferation of fibroblasts and collagen in typically small skin injuries leading to a raised scar that grows beyond the wound margins in a “claw-like” appearance |
| Exuberant granulation tissue | Formation of excessive amounts of granulation tissue (”proud flesh”) |
| Desmoid tumor | Fibrous tumors that occur during healing due to abnormal fibroblast proliferation in response to growth factors |
| Contracture | Contraction of wound edges caused by myofibroblasts. Occurs to a greater extent in healing by secondary-intention than primary intention |
Excessive healing in different tissue
| Site | Excess healing |
|---|---|
| Skin | Excessive scarring, keloids, contracture |
| Tendon | Frozen repairs |
| GIT or Urinary Tract | Strictures or stenosis |
| Solid organs | Cirrhosis, pulmonary fibrosis |
| Peritoneum | Adhesive disease |
Keloid vs Hypertrophic scar
| Hypertrophic scar | Keloid | |
|---|---|---|
| Genetics | Not familial | May be familial |
| Race | Not related to race | Black > white |
| Sex | F = M | F > M |
| Cause | Occur across areas of tension and flexor surfaces. | Abnormal fibroblasts within the wound as compared to normal dermis |
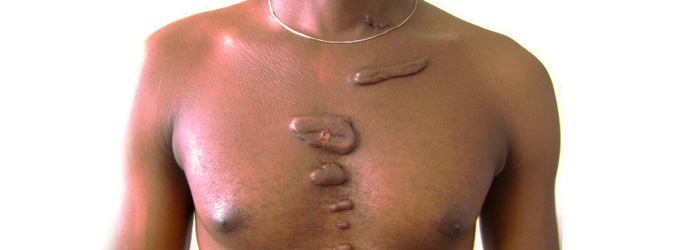
| Common site | Flexor surface, but can appear anywhere | Neck, chest, upper back, shoulders and ear lobes |
| Wound margins | Maintained, but rises above the skin level | Outgrows the wound margin |
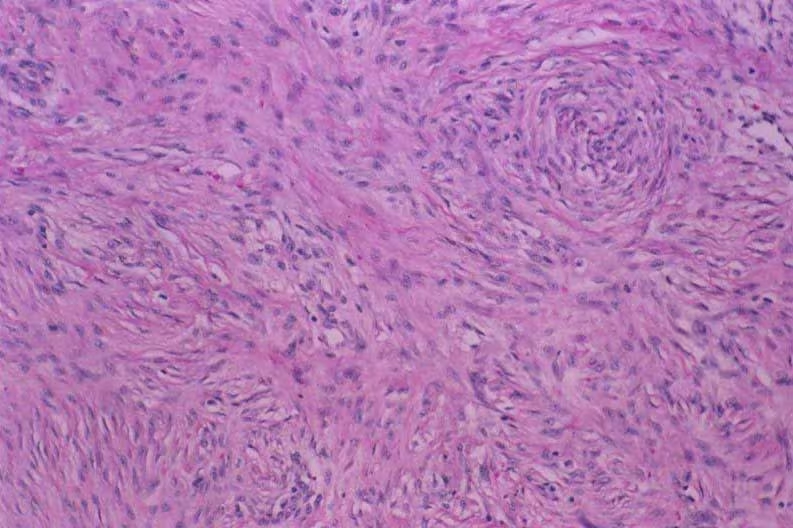
| Histology | Increased type III collagen with parallel orientation of collagen fibres | Increased type I collagen with randomly oriented fibres |
| Symptoms | Mild pruritus, but relatively asymptomatic | Pain, pruritus, hyperesthesia |
| Response to treatment | Better | Less |
| Spontaneous regression | Often | Rare |
| Prevention | Preventable with appropriate surgical incision and wound care (for trauma and burns) | No preventable |